Menu: HCH | A Vision of Health for All – Pages
Health Care for the Homeless: A Vision of Health for All
Part Four: Ongoing Work
Homelessness is likely to persist for the foreseeable future, and people without homes will need health care. The key questions posed to the presenters and participants of the HCH Pioneers Session were: In an era of expanding health insurance coverage and the broader adoption of evidence-based practices such as integrated, trauma-informed care teams, what is the ongoing role for HCH projects? How must the HCH model evolve? How can HCH help prevent and end homelessness? What is the mandate for HCH leaders moving forward?


Kevin Lindamood, president and CEO of Baltimore HCH, started off this section of the Pioneers Session by remembering when he started work there as a Jesuit Volunteer in 1993. “I got to work with this rather interesting guy named Jeff Singer. Jeff wrote the HCH Mobilizer, and in the faxed versions he embedded secret messages.” Lindamood left to go to graduate school and work in Detroit, and by the time he came back to Baltimore Jeff Singer had become the CEO, “which meant he could no longer be the Council’s policy person, which is what I think he secretly wanted to still be.” Bernie Sanders was a speaker at the National HCH Conference that year. “We were debating who gets money, who doesn’t get money from Comic Relief. Debating membership. Debating an anti-Iraq War resolution—the link between military spending and homelessness.”
Lindamood went on to say:
He concluded by stating that there are three questions to ask moving forward:
- How do we build sustainable organizations? Preparing for evolving payment models? This is a critical phase as our country wrestles with this.
- How do we build sustainable organizations that can advance deeper justice work and shape the communities around us? The importance of a living wage for our workers. Investing in our people in the long-term, so that they themselves don’t experience homelessness. The importance of consumers in deep and meaningful ways—to benefit from actual lived experiences.
- How is the policy environment we live and work in limiting us from doing the policy work we need to do? No one is acknowledging that the contemporary homelessness problem came from disinvestment in housing resources. We’re living in a toxic policy environment. How might the policy environment that we’re living in, that sustains us, that gives us the resources to do our work, how might that very environment be limiting our work in advocacy for the policy environment we need?
I think we need to reject the narrative that as a country we are ending homelessness. It’s a narrative that many of us might be participating in. It’s a narrative that we’re hearing from a lot of our partners, from federal funders—but we have to reject that narrative because we simply know it’s not accurate. I applaud HUD for finally recognizing 30 years later that housing is the solution to homelessness. We have to acknowledge that it is the disinvestment in housing that caused modern-day homelessness in the first place, and homelessness is still going to be created as fast as we can stop it.
~ Kevin Lindamood
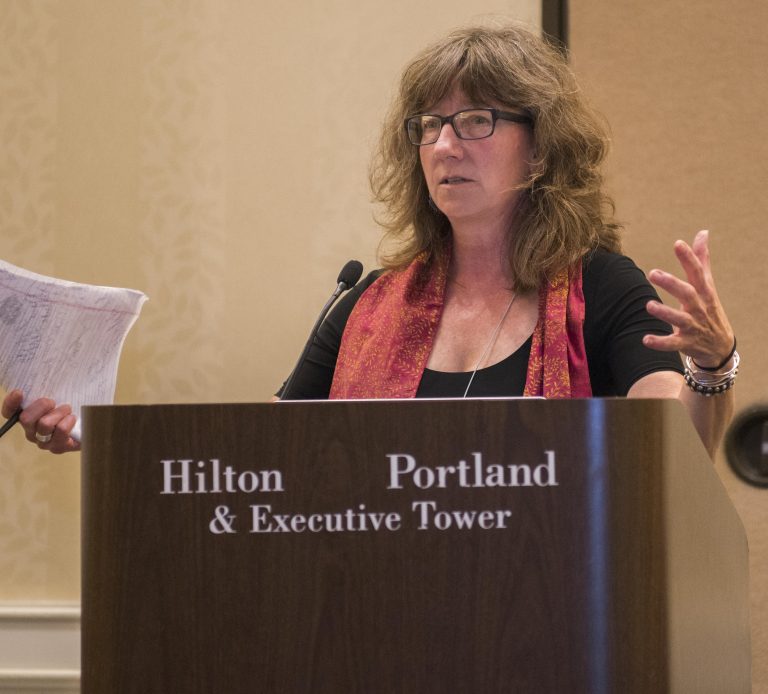
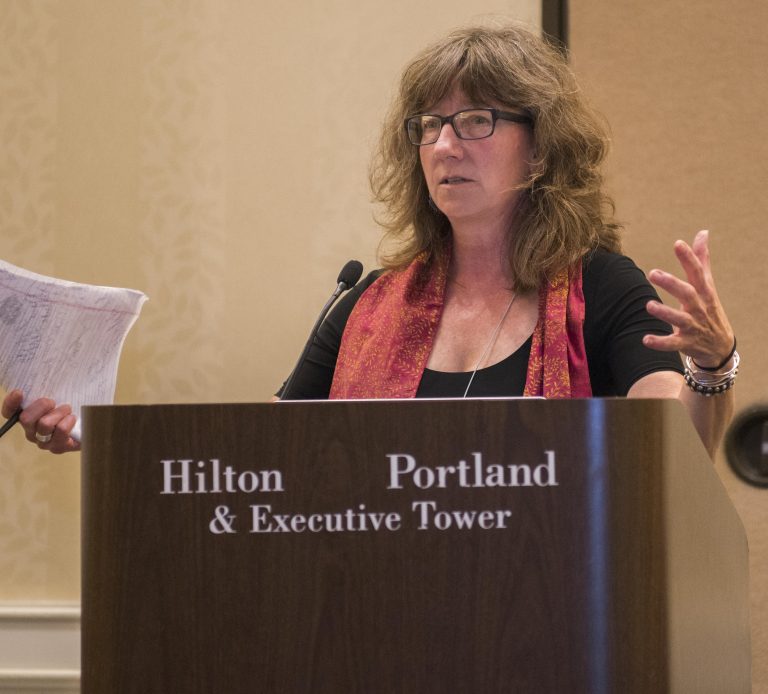
Jenny Metzler, executive director of Albuquerque HCH, spoke of how 1995 was her first HCH conference. “I cut my teeth on your stories, and I offer them up to new people. The big, righteous, smart embrace that is the National HCH Council. There’s a compendium of questions we need to ask. And how do we have these critical conversations? We need to ask ourselves the hard questions of what we aren’t doing well. Where we need to change. What we’ve done well. The inclusion of consumers, such as through the CAB leadership, but ways to bring us together even better.” Metzler went on to say, “We’re shaped by the health care environment. We can—and have also helped shape the health care environment. We’ve been a resource for the ACA. Do we shape the landscape, do we become the landscape?
Did we want to just sit back and wait for them to fail? To say, ‘I told you so’? That’s an indulgent setup to re-traumatize consumers. We’ve invited ourselves to the planning tables. We know we’re a resource. There’s strength in that identity. Pick whatever social justice issue you care about—HCH touches on it.”
Barbara DiPietro, Senior Director of Policy for both the Council and Baltimore HCH, spoke next and pointed out that she has been working with HCH for seven years, but worked 10 years before that on homeless policy. She was “drawn in by the big personalities in the cold State House—people like Kevin Lindamood and Jeff Singer. We’re at the crossroads of so many systems. I’m aware of how many allies we have. All these people we’ve touched by our values and clear dedication to our work.”
She spoke of the Medicaid work, of finding new partners through that, through health reform, which is “incremental change and not getting us where we need to go perhaps but people with power, influence, and money—they also get it now—like housing is health care—we’re not the only ones saying that anymore.” She is encouraged by the new partners in the work “who really want to get it. They’re looking for creative ways within a really complicated system, to get there. That’s a leverage point, and I’m excited about these new relationships.”
DiPietro went on to acknowledge that “we’re still working within a toxic policy environment. At the local, state, and federal levels, there’s a disinvestment in housing and social support.” She advocates the use of motivational interviewing in policy work, and for “expanding our allies—bring them in because they may be heard with a different ear. … The 51% solution[1] is a core of who we are.” She also asked, “How do we keep our values within the changing environment?” and addressed how people working within HCH never thought of themselves as mainstream. “We were scrappy, into bending rules and not asking for permission.” She also asked, “What does becoming mainstream mean? We wanted Medicaid expansion—it’s a good thing. We got what we wanted, although not for everyone.
We wanted to get our patients off the street and get them in the mainstream. There’s billing and coding—boring stuff—playing by the mainstream rules. And when we’re asked to demonstrate the value of what we do, we’re indignant that we have to do outcomes data and evaluation. … We know what we do works. The challenge is proving it through the data. … We have love and compassion. That’s an envy to a lot of folks. We can leverage that value and respect.”
She went on to call attention to the reality of people living and working within non-Medicaid expansion states. “How do we continue to support each other? I worry about the continuity of our community because we forget that not everyone is working with new resources. There are 19 states that still haven’t said ‘yes’ to Medicaid. How do we continue to support each other to get to a ‘yes’ there—so that we continue to work on an equal platform?”
Gary Cobb, a Community Outreach Coordinator for Central City Concern in Portland, Oregon, was the last panelist to speak. He talked about his work with the “quad morbidity of TBI (traumatic brain injury), addictions, mental illness, and ‘houselessness.’” He spoke of the importance of charting, of documenting TBI. He saw hospital charts of patients with “drug seeker” and “gang banger” written on them, and how stigmatizing these terms are, and that they are labels that follow patients and negatively impact their health care. “We can be instruments in how charting happens in large systems. Teams should have peer providers.”
Portland’s teams consist of peer providers, mental health professionals, addiction specialists, nurses, and housing/employment/benefits specialists. “It sounds like a big team, but it’s important to have these wraparound types of support teams.” He concluded by stating that, “Care needs to happen in a very non-judgmental way.” He developed this through motivational interviewing techniques and trauma-informed care training, as well as “reflecting on my own experience. How to provide trauma-informed care and establish boundaries—there’s a fine line there, but it can be done.”
[1] The 51% solution is a stated intention of the NHCHC to devote 51% of its advocacy efforts to addressing systemic causes of homelessness, rather than bolstering services that address the effects of homelessness.


